Martin and I were in the car. He complained he was thirsty, so I offered him a sip of my cherry-lime kombucha “soda.”
Martin examined the label, then handed back the bottle and said, “I can’t drink soda. It has refined sugar.”
“It’s okay,” I said. “It’s not real soda. It’s kombucha.”
He took the bottle again, shook his head, and said, “It says ‘cherry-lime soda.’ I’m not having any.”
I’m telling that anecdote for two reasons. First, I have read about kids who police their own food, who attend birthday parties and turn down cake and pizza. I envied the parents who could trust their kids with food choices. Now it seems I have cultivated such a kid. Martin told me recently that an assistant teacher had tried to give him a “fruit snack”—one of those corn-syrup-and-artificial-color bombs disguised as a fruit product. “I said no!” he declared, with glee. “I said I can’t have that!” Evidently he found it funny that the offer had been made at all.
Second, “cherry-lime” is a cheap way to introduce my long-promised post about Lyme disease. (Get it? Lime-Lyme? What? You’d forgotten how I promised a post about Lyme?) Lyme disease is playing a major role in our lives right now. We are fighting Martin’s Lyme disease with antimicrobial herbs, which sound innocent but provoke reactions strong, and immediate, enough for me to trace them to particular doses. On days when I want Martin to perform—say, when he’s visiting a school or completing a neuropsychiatric evaluation—I withhold or delay antimicrobials, in an effort to “even out” his behavior. It’s all so—
You’ve been on my mind.
Let’s start at the beginning. Some time ago I received this text from my mother: “I am just catching up on your blog.”—hurrah!—“Martin seems to be getting treatment for Lyme disease a lot. Does he actually have it?” Fair question. Absent an acute infection or reaction, Lyme disease is notoriously hard to diagnose. Indeed, controversy surrounds Lyme diagnosis. Some doctors, especially Lyme-literate doctors, or “LLMD’s,” have been accused of profiting by over-diagnosis and treatment. Conversely, some commentators argue that Lyme disease is at epidemic levels, wildly under-diagnosed, and mistaken for myriad other ailments. Clinical practitioners, including Doctor William Lee Cowden, who has worked extensively with Lyme disease, report Lyme prevalence levels even greater than 50% in children who present with autism. Lyme disease is a controversial topic.
I spent my childhood in Upstate New York and now live in Downstate New York, two areas where Lyme disease is widespread. In 1993, while staying in a rural area outside Berlin, Germany, I found a tick embedded in my arm, a known transmission method for Lyme and related diseases. A distant uncle of mine was hospitalized repeatedly for Lyme-related illnesses; I have a friend who lost his sister to a manifestation of Lyme disease; and my child had autism. Lyme has been on my mind for a long time.
In November 2012, Martin showed positive for Borrelia burgdorferi, the causative agent of Lyme disease, in IgG/IgM ELISA testing,. That result was bolstered by evidence of protein bands on IgG and IgM Western Blot tests. Although Lyme disease testing is not entirely reliable, Martin’s integrative physician, whom I’ll call “Dr. S,” found the evidence strong enough to recommend an extended course of antimicrobials as treatment for Lyme disease. The antimicrobials certainly seemed to affect him. For example, Dr. S recommended that I increase takuna by a few drops per day over two weeks, until Martin reached a maximum dose of 30 drops twice per day. Instead of two weeks, it took three months to reach 30 drops twice per day, because Martin reacted so strongly to each increase: crazy laughter, hyperactivity, sleeplessness.
Not long thereafter, we switched physicians because Dr. S moved to California. The new doctor, after running her own testing, said she saw no evidence of lingering Lyme infection and took Martin off the antimicrobial protocol. At the time, I was not Lyme-informed enough to know that (1) takuna and other herbs driving Martin bonkers probably meant Lyme was present and being addressed, or (2) that treating Lyme this way requires a commitment much longer than the six months we’d done the protocol.
Round two, we won’t give up.
We spent two years with the doctor who took Martin off his first Lyme protocol. February 2015, we switched back to Dr. S (all the way in California!), who took a deep breath and started trying to deal with the many issues Martin presented at the moment; the continued Lyme possibility was on the list but not at the top.
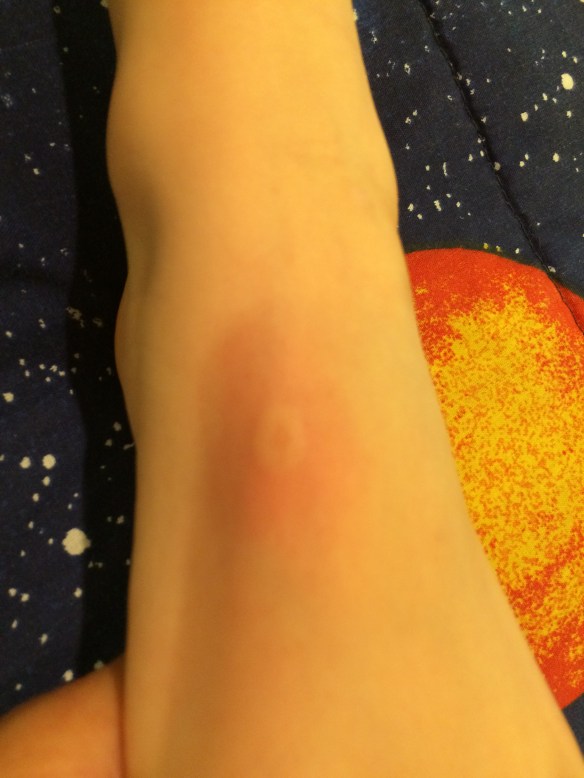
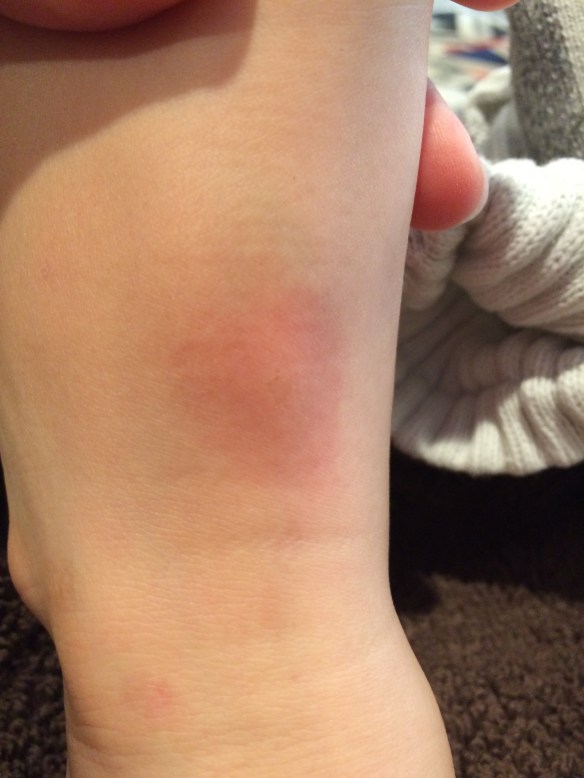
July 2015, something bit Martin on his foot, and he developed what might, or might not, have been a bull’s-eye rash. Lyme shot back up the list. With Dr. S’s approval, I took Martin to visit an LLMD in New York. That doctor had us send a blood sample to Galaxy Diagnostics in North Carolina for a “Bartonella ePCR™ Single Blood Draw” test. (If you’ve ever been present for drawing blood from Martin, you’d understand why the “Triple-Draw” test wasn’t for us.) Galaxy cultured the sample in a proprietary “Bartonella alpha Proteobacteria Growth Medium” before subjecting it to Polymerase Chain Reaction (PCR) testing. (If you’d said any of this to me before I became a biomed parent, I would have rolled my eyes.) After several weeks, the culture came back positive. Martin’s blood sample grew bartonella, a co-infection to Lyme spirochete. (The ticks that transmit bartonella also transmit Lyme, and the co-infections can be transmitted in the same bite.) Galaxy’s was the best test we could find, evidently the most definitive, and we got our answer: If bartonella flourishes when Martin’s blood is cultured, then Martin has Lyme disease.
The New York LLMD’s protocol, in such circumstances, is to put the infected patient on an extended course of antibiotics. I objected, explaining that for Martin an extended course of antibiotics could be destructive. I believe that Martin’s autism originated, in part, when he was taken from me at birth, placed in a NICU, and pumped with intravenous antibiotics. Antibiotics can kill healthy gut bacteria and thereby weaken the immune system. We have worked for years to restore Martin’s gut health and digestive functioning; I don’t want antibiotics to risk or compromise that progress. The LLMD listened to my reasoning and asked for my permission to contact Dr. S to discuss a treatment protocol.
Martin is fortunate to have these doctors. The LLMD and Dr. S ended up coordinating a phone meeting to discuss treating Martin’s Lyme disease with more natural antimicrobials versus pharmaceutical antibiotics. (Some studies demonstrate that herbal antimicrobials, or an antimicrobial/antibiotic combination, can be equally effective to pharmaceutical antibiotics alone.) In the end, Dr. S’s position carried the day, and she and the LLMD agreed on a protocol utilizing tangarana, samento, and other natural antimicrobials.
We’ve been actively targeting Lyme disease again since last October. When Dr. S adds an antimicrobial to Martin’s protocol—she substitutes the varieties in and out, to prevent the Lyme from becoming resistant—we begin a process of building to the recommended dose, sometimes as slowly as adding two drops per week. Usually, I can track the effects: When the antimicrobial stirs up too much, Martin becomes hyperactive, irritable, and unfocussed, and we need to increase more slowly.
As with nearly all facets of recovery, we see slow, steady improvement as Martin’s Lyme disease resolves. For example, Martin is holding his longest-ever independent phone conversations with Adrian, and finally eking some progress in reading comprehension. We also have tough days. This spring was a season of meltdowns and oppositional behavior. Even now, Martin is doing a lot of opposite-talking. I’m never going to use my iPad again! Never! I don’t want any dessert! Take it away! I don’t want to ride my bicycle anymore! Throw it away! He is also asking questions just to contradict the response. Do I have hockey practice today? “Yes.” No! No! No, I do not have hockey practice today. He’s not sleeping well. He’s anxious. With patience, and as much composure as I can muster, we are muddling through.
We plan to pull back, for a few months, on treating Lyme aggressively, when Martin begins his new school. That adjustment will be tough enough without die-off behavior.
Sometimes, when when ROOS strikes, the length of Martin’s recovery feels overwhelming. His autism diagnosis is gone, but he still has such trouble with attending and maintaining attention, and he is goofy and immature. Lyme disease, parasites, and the ever-present threat of candida overgrowth—will we ever finally reach the end of these issues, or will my son’s health always be an issue to “manage”?
This is our new world, right? Chronic illness for everyone.
 Martin in our pool. The lazy days of summer drag on.
Martin in our pool. The lazy days of summer drag on.
 Sunset over the docks in our little suburb. Bring on the autumn.
Sunset over the docks in our little suburb. Bring on the autumn.


 Martin in our pool. The lazy days of summer drag on.
Martin in our pool. The lazy days of summer drag on. Sunset over the docks in our little suburb. Bring on the autumn.
Sunset over the docks in our little suburb. Bring on the autumn.