Drafted in the morning, on the train, on my way to work:
Let’s conduct an experiment: How well do I understand Martin’s health these days? Can I predict what his super-knowledgable biomed doctor will say?
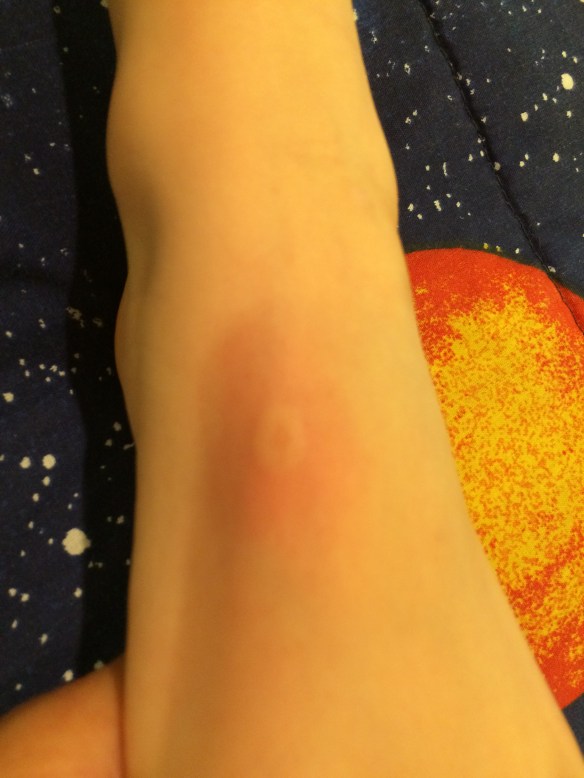
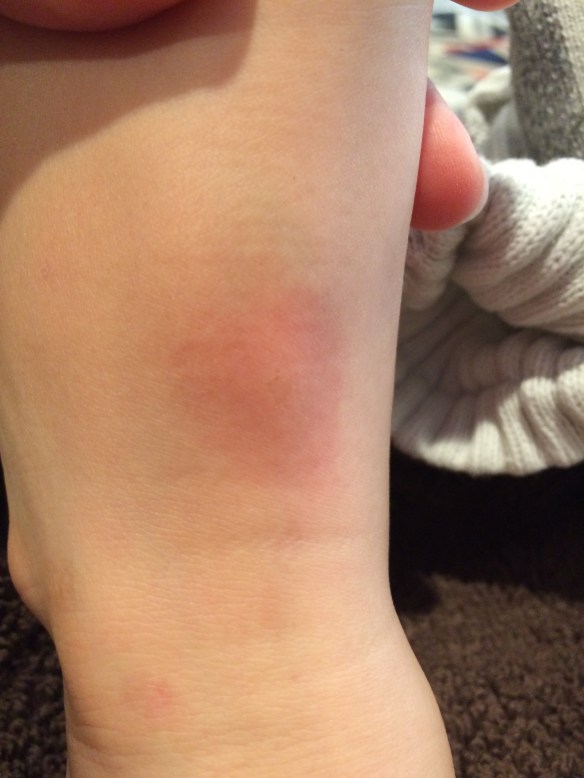
Martin is in a difficult place right now and has been for a month, ever since we last visited his biomed doctor in California, which was one month ago. Especially at bedtime, but also in spurts throughout the day, he’s beset by so much hyperactivity as to be nearly uncontrollable. The agitation and need for movement are affecting his ability to fall asleep; until nearly 10 o’clock yesterday evening, he was kicking his feet in bed, calling out, springing up to jog down the hall and return to bed. Daytimes, I’ve observed him engaging in his lone remaining repetitive behavior, which is to skip three steps pad-a-bump, run across the room, turn, stop and think (or ponder, or get lost in his own self for a few seconds), and repeat: pad-a-bump, run, turn, stop. Tuesday he did this even in our local coffee shop, pad-a-bump from the cash register to the front door, pad-a-bump back to the cash register. He’s giggly. He’s interrupting and talking over others, without regard for his surroundings. He has some increased sensitivity to sound. He’s so itchy.
Yet, as is often the case, the symptomatic behaviors seem superficial, and perhaps there is a deeper level of healing going on. He is more conversational than ever, answering questions and telling me what happens at school with minimal perseveration. His handwriting has improved dramatically; instead of gargantuan, unsteady strokes, he’s penning tight letters that actually fit on the paper lines. He’s attempting to make jokes, albeit nonsensical, unfunny ones. “I think Daddy’s going to take his hair off his head. Isn’t that funny? I’m just kidding.” He’s bargaining. “Santa Claus knows I didn’t finish my soup? That’s okay. I think Santa looks at the whole year, and I’ve had more good days than bad.” (What does he want from Santa Claus, you ask? Adele tickets. Martin has selected the most phenomenally in-demand tickets on earth and decided that’s what he wants for Christmas.)
Except for the itchiness, which predated our last visit to California, the hyperactivity, repetitive behaviors, and other symptoms began, as near as I can reckon, right when we returned from that trip, one month ago. The sequence was like this: Thursday afternoon we flew from New York to California. The flight was delayed, and Martin wasn’t in bed until 11:00 pm PST, or 2:00 am EST. He managed to sleep until 9:00 am PST, or noon EST. We spent Friday afternoon at the doctor’s and, as part of that appointment, Martin had an LED treatment. Friday evening we met friends (a father and his son, Martin’s age) for dinner, which went well. Martin fell asleep around 10:00 pm PST Friday night and slept well. Saturday was a packed day. We went out to breakfast, and then to see my friend’s new house, and then we drove inland an hour, to spend the afternoon with the same friend’s mother and to visit George the cat, who now resides on the West Coast. It was 6:30 pm when Martin and I returned to our hotel.
That night, Saturday night, our placid California weekend went awry. Martin knew we had to get up early (3:45 am) to drive 40 minutes to the airport, return our rental car, and catch the 7:00 am flight to New York. He was excited about getting up so early. Too excited. He went to bed giddy around 8:00 pm and—I don’t have a better way to put this—worked himself into a frenzy, calling out, laughing, asking whether it was time to get up. Around 9:30 pm, anxiety took over. Mommy! Mommy! Something is wrong! Mommy! I don’t know what’s going on. Mommy, where are you? [I was in the same hotel suite, using my iPad, where he could hear me and see the light I was using.] Mommy, help! Help me! His agitation mushroomed until he was sobbing and even shrieking. In an effort to calm him, I said, unthinkingly, “Martin, you have to stop. You have to stop screaming. We are in a hotel. Someone could think I’m hurting you and call the police!” That foolish statement became a target for his previously unspecific anxiety. Are the police coming? Are the police here? Will the police take me away? No! No! Mommy, tell the police not to come! I don’t want the police to come!
My poor little man was terrified and out of control. At last I took him to my bed, climbed in, and squeezed him until he began to calm. Once the sobbing reduced to whimpers, I released him and rubbed his head instead. Within two minutes from that point, he was sound asleep and I had quiet time to wonder what the hell had just happened.
When I woke Martin at 3:45 am, after just five hours’ sleep, he sprang from bed, evidently cheerful to be getting up at such a special time. I saw no trace of anxiety or giddiness. That day, Sunday, as we traveled home, he seemed restless and uncomfortable, which I chalked up to lack of sleep, but otherwise unremarkable. Sunday evening, however, he became hyperactive and had trouble getting to sleep.
Since that Sunday evening, we’ve endured the hyperactivity, some inappropriate laughing, continued itchiness, and lack of focus. Charcoal tablets help, but not always. We’ve started a new protocol of supplements, antimicrobials, homeopathic remedies, and yeast fighters; I’ve introduced the new elements slowly, and haven’t tied a specific reaction to any. Last week for Heilkunst we cleared a DTaP vaccine, again without a specific reaction, only the same hyperactivity. The hyperactivity is uniformly worst at bedtime, and Martin continues having trouble getting to sleep. He’s woken early a few times but generally sleeps through the night.
So what is going on here?
I have scheduled a short call with the doctor this afternoon. I’m going to write what I think is happening, and then, after I speak with the doctor, I will give her thoughts. I’m eager to see whether we agree.
My own theories: First, I think yeast is at work. I said, even before we went to California, that I believed Martin was suffering a yeast flare. The poor kid is so itchy. He’s scratched his legs and belly bloody. He’s giggly and “drunk.” Second, I wonder whether the LED he had in California might have kicked up some toxins that Martin is having trouble clearing. Maybe?
Drafted the next day, after I spoke with the doctor:
The doctor disagreed with my guesses. While yeast might be a subsidiary issue, she said, Martin’s hyperactivity makes it unlikely that yeast is the primary issue. Hyperactivity has not been a hallmark of Martin’s previous yeast flares, she pointed out. As to the LED, she said that any effects would have emerged during the 25 hours immediately following the treatment. Saturday night, when Martin experienced the anxiety attack that launched this hyperactive period, some 30 hours already had passed.
She admitted that it’s tough to know exactly what’s going on. Her theory: Banderol and borrelogen, the antimicrobials that Martin has been taking in incrementally increasing doses to treat chronic Lyme, are too strong. His sensitive system needs time to adjust. She reminded me that, when we used banderol three years ago, as well as when we used the antimicrobial takuna, we had to increase the dose extremely slowly—sometimes by not more than one additional drop per week. This go-round I’ve been building banderol and borrelogen by about a drop per day each. She asked me to hold the antimicrobials for 48 hours (or four doses, as we dose them twice daily) and she if Martin’s hyperactivity decreases.
I was going to post this blog entry after taking to the doctor. Now I feel like it’s worth waiting another couple days to announce the results of our 48-hour experiment.
Drafted two-and-a-half days after I spoke with the doctor:
Better. Around 6:20 am I messaged the doctor:
I think you nailed the issue. Since we spoke on Thursday, I have withheld banderol and borrelogen (so five doses withheld so far: Thursday evening, Friday morning and evening, Saturday morning and evening). We have seen a perceptible, marked decrease in Martin’s hyperactivity, and Friday night he was able to go right to sleep for the first time in weeks. Yesterday afternoon I took Martin into the infrared sauna for a detox cycle. Going in the sauna really, really agitated him. For an hour or so, the hyperactivity was back, full-force, and then we had some emotional dysregulation. On the other hand, last night Martin went right to sleep again, his pre-bedtime meltdown notwithstanding. What do you suggest? BTW, we have continued during this time with four drops Clovanol daily. Thank you!
Pretty intense, right? And I didn’t even tell her that he had flat-out refused to watch Pride and Prejudice with me on the sauna video screen. “Turn it away from me!” he said. “I don’t want to see it!” That evening, I messaged the doctor again:
An additional note: Today (Sunday) the hyperactivity was back up again, though not as bad as before. We haven’t restarted banderol or borrelogen. Today Martin also was “floppy” (this could be the lack of MitoSpectra) and emotionally volatile—he had a meltdown over where we chose to have Sunday dinner, and was not able to recover for quite some time. He’s in bed now, making noise instead of going to sleep. I’m wondering if yesterday’s sauna has lingering effects.
She responded by advising me to continue holding banderol and to restart borrelogen from one drop per day, or even one drop every other day, and build even more slowly than before. She also suggested that I keep Martin out of the infrared sauna for a while, as it may be too intense and also stirring up metals. Regarding the floppiness, she advised putting Martin back on mitochondrial support immediately, and said that might also help him better handle the antimicrobial herbs.
Drafted four days after I spoke with the doctor:
Hyperactivity is reduced again. Unfortunately, emotional dysregulation is taking hyperactivity’s place. (That’s a kind way to say that Martin is moving less but melting down more.) Also, Martin is distracted. This could be simply a result of the changes in his antimicrobials, and the fact that his new MitoSpectra hasn’t yet arrived. Here’s hoping that he evens out soon.
Note for careful readers:
Are you wondering why Martin has been off MitoSpectra? I knew it. You are very careful readers. The last two bottles of MitoSpectra I purchased went bad; the pills changed color and developed a fishy smell. I became nervous about continuing to use the product. But I do like MitroSpectra and believe it’s been helpful to Martin. After talking with a representative of the company, I’ve decided to give I decided to give it another shot. Help us, MitroSpectra!